The Joy of 50 Years: Neuropathy, Gut Ache, Gallbladder Polyps
Update 2014-02-02: right side pain has been gone for 10 days. Polyps can stay for now, will recheck in 6-9 months for stability. Neuropathy healing.
In spite of the nerve damage (Metronidazole (Flagyl) antitiotic reaction (autonomic neuropathy), I had an exceptionally strong training week around the last week of the year. A full week of very strong 2+ hour rides felt great. The Bad makes the Good even more delicious.
I had hoped that given a few weeks my body would steadily heal the nerve damage. But while the initial symptoms abated, it now seems to be regressing: no overt tingling but low level pinprick sensations in hands, a feeling of weakness in forearms, odd little sharp pains in wrists and forearms as far as the elbow, gritty feeling toes that have blotchy discolored purple areas. Not so pleasant, but all pales in comparison to the prospect of no improvement, or the disheartening prospect of worsening symptoms, or a propensity to further damage by unknown future agents.
Blood sugar
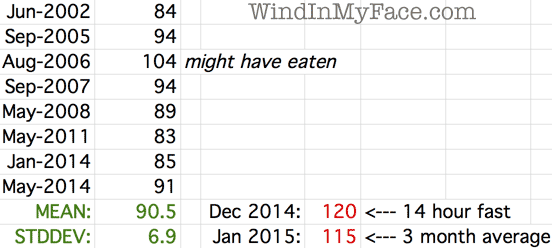
Equallly worrisome is that my blood sugar which for 12 years tested (fasting) in the low 80's to 90's historically, was tested in late December at a whopping 120 (14 hour fasting), then retested in January at 111 as a 3-month average (blood test for average glucose based on red blood cells).
I seem to be a statistical data point in a case-plot band to doctors, who seemingly consider a radical outlier (in standard deviation terms) as “normal”, because it falls just short of diabetic. Perhaps damage from the Metronidazole might not be limited to neurological effects. Or it could be something else. But my glucose was normal (85) in May 2014 in the midst of the right side gut ache issue, so that suggests some other precipitating cause. Like the neuropathy, the future prospects look uncertain. And I have felt like I’ve been carrying extra fluid for some months now; this might be related to blood sugar.
Right side gut ache / bloating vs gallbladder
The right-side gut ache (now a 9 month ordeal) for which I took the damned antibiotic is back with a vengeance for over a week now along with uncomfortable bloating and an enervating energy drain. So while I’ve continued training, my power meter reading say it lops off 10-15%. I've had to cut back, but that isn’t solving anything—I just feel marginal when I don’t get exercise. Recovery is also impaired; whatever the root cause, that right side gut ache and bloating is exacting a significant “energy tax”.
Because the right side pain increased to a level that could not be ignored for long, I went in for an ultrasound for the gut. As an “incidental finding”, 3mm polyps were found in my gall bladder. All doctors I consulted indicate that that gall bladder ought to come out, even forgetting other symptoms. And all agree that it might have nothing to do with the right side ache / bloating symptoms, or that it might be the root cause. No one can say.
“There are multiple gallbladder polyps measuring up to 3mm. No gallstones or sludge. No gallbladder wall thickening or pericholecystic fluid to suggest cholecystitis”.
So next up is Laparoscopic Gallbladder Removal (Cholecystectomy). I’m going to find a very experienced surgeon, as I don’t want the common bile duct damaged or bruised.
Another possibility
Besides the gallbladder, another possibility for the right-side ache could be sphincter of ODDI disfunction.
Individuals with sphincter of Oddi dysfunction present with abdominal pain resembling that of structural or inflammatory disorders of the gallbladder, biliary tree or pancreas. Among other characteristics, the pain is typically in the upper part of the abdomen or in the right upper quadrant of the abdomen, lasts 30 minutes or longer, and is not associated with a structural abnormality that could lead to these symptoms.
Functional disorders of the gallbladder, bile duct and pancreas have been defined and classified by the Rome criteria for functional gastrointestinal disorders.[2] The criteria outline three variants of functional disorders of the gallbladder, bile duct and pancreas, termed functional gallbladder disorder, functional biliary sphincter of Oddi disorder and functional pancreatic sphincter of Oddi disorder. All of the following criteria need to be met for as part of the definition of a functional disorder of the gallbladder:[2]
- the pain must be located in the upper part of the abdomen and/or the right upper quadrant of the abdomen
- episodes of pain must last at least 30 minutes
- the symptoms must be recurrent, and occur at differing intervals
- the pain must incrementally increase to a "steady level"
- the pain must be severe enough the patient's daily activities are affected, or that the patient must attend the emergency department
- the pain must not be relieved by any of bowel movements, change in posture, or antacids; and,
- other structural disorders that could explain the symptoms must be excluded.








